
Thank you: Hotzevitamins.com

Thank you: Hotzevitamins.com

A true glow-getter, Honey-Dip offers both the perfect sun-kissed glow and anti-aging benefits in one convenient bottle. Delivering intense hydration and nutrient support for youthful and clear skin, this healthy alternative to typical self-tanners is chemical free and infused with organic ingredients, pure botanicals and naturally derived DHA for a decadently radiant complexion.
 First off, Exfoliate
First off, Exfoliate The right formula and tone
The right formula and tone
 Smear with no fear
Smear with no fear Take your time drying
Take your time drying Make your color last
Make your color last

This is a guest post by Laura Schoenfeld, a Registered Dietitian with a Master’s degree in Public Health.
One of the downsides of using “the Pill” is that many times it’s hard to get back to a normal menstrual cycle once you stop taking it. Some of my young female clients in their 20s and 30s who were taking birth control for a long time and then stopped haven’t had their periods for months, or sometimes even years!
It can be frustrating, especially for women who have stopped taking birth control because they want to become pregnant. And my clients realize that having amenorrhea isn’t a good sign for their overall health regardless of their childbearing plans, so they’ve come to me to help them make the diet, supplement, exercise, and lifestyle changes they need to in order to get their hormones back on track.
Has birth control use made you lose your period? Get it back naturally with these tips by @AncestralizeMe!
Since this is a common experience for women my age, I wanted to share my best suggestions for recovering from post birth control syndrome using diet and lifestyle, in order to help those who have been frustrated by the symptoms associated with the condition. The following are tips you can follow without needing a doctor’s visit or a prescription. Read on to learn how to get your period back!
As a dietitian/nutritionist, nutrition is always the number one focus in any of my health improvement plans. My clients who’ve aren’t having regular periods tend to be some of the fastest responders to a tailored nutrition and supplement program, primarily because the loss of menstruation is often be a sign of underlying nutrient deficiencies. Even if you’re eating a whole foods, Paleo diet, there are many nutrients that can be inadequate if you’re not making a concerted effort to include specific foods and/or supplements.
There has been evidence accumulating over the years that certain nutrients may become depleted while a woman is on an oral contraceptive. While there are likely dozens of nutrients that are important in regaining your fertility and monthly cycle, there are a few in particular that I find to be extremely effective in helping to recover the menstrual cycle.
Zinc is a critical nutrient to consider, and many nutritionists recommend an increase in zinc intake for female clients struggling with loss of menstruation following the use of the Pill. There is evidence demonstrating that women who take oral contraceptives have lower plasma zinc levels, so they may have higher need for this important mineral for fertility.
Some healthcare practitioners theorize that taking oral contraception might either cause zinc deficiency or even copper overload, which could contribute to the loss of healthy menstrual function. Either way, I always include zinc as part of my recommendations for my clients with amenorrhea.
Zinc can be sometimes difficult to replenish without short term therapeutic supplementation, even in the context of a whole foods diet. If you’re willing to eat lots of shellfish (e.g. oysters and clams), red meat, pumpkin seeds, and poultry, you may be able to avoid supplementing with zinc in this case. I usually recommend 15-30 mg of zinc per day for someone with post birth control syndrome. (If you do supplement, be sure to take it with a meal, otherwise you may get sudden, intense nausea.)
Magnesium is another mineral that I find beneficial for my clients with post birth control syndrome. While many of us in the ancestral health community feel that everyone can benefit from daily magnesium supplementation, it’s especially important for those on birth control (or coming off birth control) to supplement with magnesium.
Magnesium is difficult to get enough of in our modern diets, and some evidence shows that serum magnesium levels are reduced by oral contraceptive use. If you have a history of birth control use, I recommend using a chelated form of magnesium and taking 200-400 mg daily to supplement what you’re getting from food.
Finally, vitamin B6 is another nutrient that is not often discussed but can be very helpful in restoring menstrual function in those with post birth control syndrome. A 2011 study found that those who used oral contraceptives had lower plasma vitamin B6 concentrations, and one type of amenorrhea caused by high prolactin levels was able to be treated using B6 supplementation, suggesting that supplementing with B6 may be beneficial in post birth control syndrome.
Vitamin B6 is found in a variety of foods, and is generally safe to take as a supplement at doses below 100 mg per day. I like Designs for Health’s Sublingual Vitamin B6, which has the added benefit of providing a small amount of chelated zinc. At 50 mg per teaspoon, it’s a high enough dose to replenish any depleted stores, but not so much to risk toxicity with long term use.
There are other nutrients that I address with my clients, either making diet or supplement recommendations to address potential deficiencies in their diets. One nutrient that I find tends to be quite low in many of my young female clients’ diets is vitamin A. You can get plenty of vitamin A by eating 4-8 ounces of beef or lamb liver every week, and that’s almost always something I recommend to my clients who are struggling to regain their periods. Another important nutrient is vitamin D, which typically comes from adequate sun exposure but can be helpful as a supplement for those with blood levels below 30 ng/mL.
There are many nutrients that may be negatively affected by long term birth control use, and every person’s needs are unique. If you’re struggling with post birth control syndrome and aren’t sure if your nutrition has been optimized for your recovery, I recommend working with a knowledgable nutritionist who can help assess your diet for possible nutrient gaps.
This suggestion might sound a little off the wall, but hear me out: in our modern world of late night TV, attachment to our cell phones, 24 hour artificial light, and inadequate hours of sleep, our circadian rhythms have taken a serious beating.
Circadian rhythms are physical, mental and behavioral changes that follow a roughly 24-hour cycle, responding primarily to light and darkness in an organism’s environment. People who fly across several time zones experience circadian rhythm disruption as “jet lag”, but even less dramatic shifts in your circadian rhythms can cause significant health problems, including infertility and amenorrhea.
Your circadian rhythms affect all endocrine hormone secretions, including melatonin, cortisol, thyroid stimulating hormone, growth hormone, prolactin, follicle stimulating hormone (FSH), luteinizing hormone (LH), insulin, leptin, and more. (1) While we don’t know how all of these hormones might contribute to healthy menstruation, we do know that prolactin, FSH, and LH are the key hormones regulating the menstrual cycle along with estrogen and progesterone.
So it’s not a stretch to assume that if these hormones aren’t being released at the appropriate times, the reproductive system won’t be getting the proper signals that are needed to regulate the menstrual cycle. And some research does show that circadian rhythm disruption from jet lag and shift work can wreak havoc on women’s reproductive function. (2)
There are dozens of factors that affect circadian rhythms, but I’ll just focus on the two most important: light exposure and sleep. Proper light exposure includes getting adequate daytime sunlight and appropriate elimination of bright light at night. The biggest influence is the light hitting your eyes, so I strongly suggest making an effort to get outside, or at least sit by a window, for most of the daylight hours. On the flip side, you also need to ensure you’re not getting blue light exposure once the sun has gone down.
There are ways you can address this issue even if you can’t go outside during the day or shut off all your lights when the sun goes down. The first is to get a light therapy lamp that can help provide the right spectrum of daytime light during your day, which you can set up at your work desk. The second is to block blue light at night, and the easiest way to do this is by using these super fashionable orange goggles. You can also use orange light bulbs as your evening lighting option.
And of course it should go without saying that you need to prioritize your sleep, going to bed early enough to get a full 8 hours of sleep every night.
This is one of the most difficult recommendations for many of my clients, as frequently those dealing with post birth control syndrome are also trying to lose weight. And more often than not, their weight loss attempt includes reducing their food intake and cutting down on carbohydrates.
While this strategy may help with short term weight loss, it’s definitely not conducive to your hormonal health to significantly limit your food intake in this way. It’s a well known phenomenon in the medical world, called the Female Athlete Triad, where women under eat and overtrain so much that they lose their menstrual function, and even put themselves at risk for osteoporosis.
Stefanie Ruper has written a fantastic article on the problems with being overly restrictive with your food intake, and how dozens of her readers have written to her complaining that they lost their menstrual function when switching to a Paleo diet. She acknowledges that it’s not the Paleo diet that is the issue per se, but that those who switch to Paleo often get stuck in an overly restrictive, low carbohydrate approach that does not support healthy endocrine function through various effects on the HPA axis and thyroid hormone conversion.
I think it’s safe to say that those women dealing with post birth control syndrome should also be wary about how restrictive their diet is, and ensure that they’re getting enough calories and carbohydrates to support their activity levels. I generally recommend at least 20-30% of calories from carbohydrate for my patients who aren’t getting their period, and provide them an appropriate calorie range for their body size and activity levels. Trying to quickly lose weight while dealing with amenorrhea is rarely a good combination.
And the other side of this issue is avoiding overtraining, which is another problem I see in many of my young female clients trying to “lean out”. As I mentioned, this overtraining and undereating combination is known as the Female Athlete Triad and is well known as a cause of amenorrhea. Overtraining means different things to different people; what might be a normal training schedule for an elite athlete may cause burnout and hormonal disruption in a non-athlete. If you’re dealing with amenorrhea, you need to take a serious look at your training regimen and make sure you’re not overdoing it.
This is another big issue for many of my young female clients experiencing amenorrhea. Stress is generally unavoidable in our modern lives, but that doesn’t mean you have to let it disrupt your life and throw off your hormone regulation.
Chronic stress causes hypothalamic‐pituitary‐adrenal (HPA) axis dysregulation, which is also known as adrenal fatigue. (3) Unfortunately, the hypothalamus and pituitary gland are also key regulators of the menstrual cycle. (4) Thus, chronic stress is easily able to cause irregular menstrual cycle activity, and can even lead to a condition known as hypothalamic amenorrhea. This is very similar to what happens in the case of the Female Athlete Triad, and is typically caused by the chronic physical and/or emotional stress that is unfortunately common among young women.
For those trying to overcome post birth control syndrome (or any type of amenorrhea for that matter), getting stress under control is very important. This includes the recommendation above regarding eating enough and avoiding overtraining, but it also deals with managing daily stress from work, relationships, financial issues, and more.
I always tell my amenorrheic clients to find a stress management protocol that works for them, which can include yoga, meditation, journaling, deep breathing, and more. Anything you enjoy doing that helps relieve stress is a great choice, and can make a big difference in your return to normal menstrual function.
Having a strong ability to detoxify is crucial for recovering from post birth control syndrome, as one of the primary issues with taking oral contraceptives for a long period of time is hormonal build up. Your body stores hormones like estrogen in your fat cells, and these stored hormones can linger for months or years after you stop taking the Pill. Your liver is responsible for clearing these hormones through the bile, and if you’re not detoxifying well enough, your liver is ineffective at eliminating these excess hormones.
There are many ways to boost detox capacity – too many to get into in this article – but one great supplement that can help improve your detox capacity is Chris’sPaleologix AdaptaClear, which contains a variety of B-vitamins, amino acids, and herbal extracts that support the body’s natural detoxification process. In addition, I’ve written another article in which I recommend increasing intake of certain foodsthat can help boost hormone clearance.
And wouldn’t you know it, your gut flora can even help you detoxify excess hormones. This podcast I’ve linked to is all about the “estrobolome,” the complete set of bacterial genes that code for enzymes capable of metabolizing estrogens within the human intestine. (5) So taking a high quality probiotic and eating fermented foods, especially fermented cruciferous vegetables like sauerkraut, is an important part of recovering from post birth control syndrome.
These are my best general recommendations for how to regain your period after stopping birth control, and I’ve used these strategies successfully with many young female clients. It’s important to address all these factors, as any one of them can be enough to disrupt menstrual function, which is a sign of suboptimal health.
Of course, sometimes this isn’t enough to get you back on track hormonally, especially if you were taking birth control for many years, or if you started birth control as a method to address hormone issues in the first place. In this case, you may need some additional testing done to identify any issues that may be causing your amenorrhea. PCOS is a very common condition that can significantly disrupt your hormonal function, so you’ll want to discuss this possibility with your endocrinologist.
And of course working with a knowledgable nutritionist can help you identify the missing pieces in your recovery plan to ensure that you’re doing everything possible to get back your hormonal health and menstrual function.
Now you tell me – have you ever struggled with post birth control syndrome and/or amenorrhea? What helped you get your period back? Share your story in the comments below!
 About Laura: Laura uses her knowledge of traditional and biologically appropriate diets to improve her clients’ health. Growing up with a family that practices Weston A. Price principles of nutrition, she understands the foods and cooking practices that make up a nutrient dense diet.
About Laura: Laura uses her knowledge of traditional and biologically appropriate diets to improve her clients’ health. Growing up with a family that practices Weston A. Price principles of nutrition, she understands the foods and cooking practices that make up a nutrient dense diet.
With her strong educational background in biochemistry, clinical nutrition, and research translation, she blends current scientific evidence with traditional food practices to help her clients determine their ideal diet.
You can find her at AncestralizeMe.com, on Facebook, and Twitter!




 We've been fighting for years against nasty ingredients in our foods—avoiding trans fats, spurning high-fructose corn syrup, steering clear of pesticides in our produce and antibiotics in our meat. Now we're facing the most serious battle yet, against insidious toxins in our food that haven't been measured or quantified; in many cases, they can't be avoided.
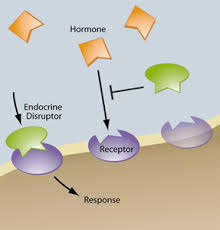
We've been fighting for years against nasty ingredients in our foods—avoiding trans fats, spurning high-fructose corn syrup, steering clear of pesticides in our produce and antibiotics in our meat. Now we're facing the most serious battle yet, against insidious toxins in our food that haven't been measured or quantified; in many cases, they can't be avoided.These toxins, collectively called endocrine disruptors, are present in nearly every aspect of our environment—not only food, but also personal care products and household goods. Endocrine disruptors are a broad category of chemicals that interfere with the normal functioning of the endocrine system and can create imbalances throughout the body, particularly in the thyroid, reproductive, and adrenal systems. More than 50 different chemicals—found in herbicides, pesticides, fertilizers, plastics, food preservatives, personal care products, meat and dairy, and more—are known to act as endocrine disruptors, says Ann Louise Gittleman, PhD, CNS, author of Before the Change: Taking Charge of Your Perimenopause.
Xenoestrogens, one of the more troubling types of endocrine disruptors, mimic estrogens and attach to the body's estrogen-receptor sites, in both women and men. These xenoestrogens interfere with hormonal signaling and are believed to cause an increased risk of breast, prostate, and reproductive cancers; reduced fertility; early puberty in children; menstrual irregularities; endometriosis; and other disorders. A new area of research is now pointing to the obesogenic effects of xenoestrogens and other endocrine disruptors: chemicals that disrupt our hormones are also making us fat, says Bruce Blumberg, PhD, professor of developmental and cell biology at the University of California, Irvine.
That's not to say the die is cast. You can't change your past, but you can change your future. Here's how.
We thought if we kept the Tupperware out of the microwave and used only natural deodorants, we were safe from xenoestrogens. Boy, were we wrong! These toxic compounds are everywhere. Here's your room-by-room rundown for eliminating xenoestrogens, starting with the kitchen:
THE PANTRY. Start with your food shelves. Most processed food contains some kind of undesirable material, says Blumberg, either in the packaging itself or the ingredients. Canned foods are usually packed in cans lined with plastic coating that contains bisphenol-A (BPA), a xenoestrogen. According to an Environmental Working Group (EWG) study, chicken soup, infant formula, and ravioli had BPA levels so high that just one to three servings could expose a woman or child to BPA at levels that caused serious adverse effects in animal tests. Cut back on processed and packaged foods in general, and choose packaged goods in glass or paper containers. Buy grains, nuts, dried fruits, and beans in bulk, and store in glass or stainless steel containers.
THE REFRIGERATOR. Are your milk and burgers organic? If not, they may contain synthetic estrogens, which are used to make cattle grow bigger faster and to increase their milk production. Pesticides on the food the animal eats may also contain xenoestrogens, which can be concentrated in the animal's fat, flesh, and milk. Produce should also be organically grown; anything that's not may contain insecticide or pesticide residues, which can have estrogenic effects, says Blumberg. Buy only organic meat, dairy, and produce, locally whenever possible. If you can't buy all your produce organic, check the EWG's Dirty Dozen list of the most contaminated varieties of fruits and vegetables at foodnews.org and choose low-fat meat and dairy products. HDPE and LDPE (high- and low-density polyethylene) plastics, Nos. 2 and 4 respectively, are hard plastics that are used to make milk jugs and some water bottles. These plastics are generally safe and do not react with the contents of the container.
COOKING AND PLASTICS. You may already know not to heat food in a plastic container, since heating some plastics can cause xenoestrogens to leach out of the container and into the food. But did you know Styrofoam containers contain BPA and that drinking coffee out of a Styrofoam cup causes the BPA to leach out? The moral: never microwave food in anything other than a glass container or on a paper towel. Another source of xenoestrogens comes from Teflon-coated nonstick pans, which if overheated can release endocrine-disrupting perfluoroalkyl compounds, says Blumberg.
FOOD-STORAGE CONTAINERS. Trash your Tupperware and replace it with glass or stainless steel food-storage containers. Or stash food in small glass or metal bowls covered with a saucer. Some plastic cling wrap is made from PVC (polyvinyl chloride), which contains several types of xenoestrogens and other endocrine disruptors, says Blumberg; PVC can leach out, and should never touch food. If possible, buy your (organic) cheese cut to order from the deli, and have it wrapped in plain, uncoated paper; most butcher's paper has a shiny, waterproof PVC coating. Otherwise, shave off any parts that have touched cling wrap, and store the cheese in a glass container or wrapped in paper.
THE KITCHEN SINK. Tap water can contain xenoestrogens from medications and agricultural and chemical pollution. Bottled water isn't always a good solution, since it's usually packaged in flexible plastic that contains phthalates, known endocrine disruptors. Most bottled water is sold in No. 1, (PET or polyethylene terephthalate) plastic containers. However, HDPE and LDPE plastics are safe for drinking water. If you're refilling your hard plastic water bottles at the grocery store, they're probably made of polycarbonate (No. 7), which contains BPA, says Blumberg. Best solution: buy a high-quality activated-carbon water filter, and if you must store your water, use glass bottles.
THE BATHROOM CABINETS. Sadly, one of the most effective ways to absorb xenoestrogens is via the skin. Lotions, creams, makeup foundations, nail polish, deodorants, and other personal care products may contain xenoestrogens in the form of parabens, phthalates, and other compounds. Use only personal care products and nail polishes that are clearly marked "paraben free." And if you're using nonoxynol-9 spermicide as your birth control method, find a more natural method; nonoxynol-9 breaks down in the body into xenoestrogenic nonylphenols.
THE BATHROOM SINK. Your toothbrush and bathroom cup are probably made of plastic. As long as you're not eating the toothbrush handle, you're OK. But ditch the cup unless it is No. 2 or 4 plastic, and use a glass or stainless steel one instead. As for toothpaste, it may contain parabens and other xenoestrogens. And the soap or gel you're using to wash your hands and face? You guessed it. Buy chemical-free versions of both.
THE SHOWER. Guess what? Your shower curtain is probably lined with flexible vinyl that contains phthalates, and may contain mercury, dioxins, and lead. Shampoos and conditioners usually contain parabens and other xenoestrogens; a few are made with added estrogen. Use cloth shower curtains or a sliding glass door, and check ingredients on hair care products.
THE BABY'S ROOM. Children are the most sensitive to xenoestrogens and other endocrine disruptors; sadly, any room belonging to children may be filled with xenoestrogens. Baby bottles can be made of rigid No. 7 plastic that contains bisphenol-A. Flexible plastic bottle liners should be made from No. 4 LDPE plastic. Many plastic toys contain phthalates, and flame retardants used in children's clothing are xenoestrogens, says Blumberg. If you do not know what type of plastic it is, don't give it to a child who may put it in her mouth. Consider buying wooden, fabric, paper, and metal games and toys.
THE LAUNDRY ROOM. Dryer sheets are loaded with xenoestrogens that permeate clothing and come into direct, prolonged contact with the skin. Same goes for laundry detergent. Buy only the chemical-free varieties. Skip the dryer sheets altogether, and use natural liquid fabric softener in the rinse cycle. Or try adding 1/2 cup of baking soda to the rinse cycle for softer laundry.
THE BACKYARD. Home lawn care products such as pesticides and weed killers may act as xenoestrogens. In one study, atrazine, a commonly used weed killer, affected animals at doses as small as 0.1 parts per billion. Use the natural versions, or learn to live with weeds.
Fight Back with Nutrition No matter how diligent you are in removing xenoestrogens from your home, you'll still encounter them in the outside world. Meanwhile, you've certainly been exposed to xenoestrogens sometime in your life. The task, then, is to protect the body from their harmful effects. Certain foods and herbs can shield estrogen receptor sites so xenoestrogens can't attach, help the body metabolize and excrete harmful estrogen, and protect the body from xenoestrogen damage, says Jillian Michaels, a trainer for television's The Biggest Loser and author of Master Your Metabolism. Some of the best:
BROCCOLI, CABBAGE, KALE, BRUSSELS SPROUTS, AND OTHER CRUCIFERS are rich in indole-3-carbinol (I3C), which the body converts to diindolylmethane (DIM), says Shari Lieberman, PhD, CNS. DIM then induces certain enzymes in the liver to block the production of the toxic estrogens and step up the production of the beneficial forms. The best way to eat them is lightly steamed to protect I3C levels or, better yet, pickled: some studies have attributed the low rates of breast cancer in Polish women to their high daily consumption of sauerkraut. Crucifers are also high in sulforaphane, a powerful breast-cancer inhibitor. Best protection: add steamed broccoli to salads; roast cauliflower and Brussels sprouts in olive oil; try sauerkraut or kimchee, a spicy fermented cabbage. Supplements of I3C are available at health food stores; a typical dosage is 150–300 mg per day.
FLAX is the richest source of secoisolariciresinol diglycoside (SDG), a compound that the body converts into lignans, says Michaels. Lignans are phytoestrogens and help balance the body's estrogen levels by binding to the same estrogen receptor sites that xenoestrogens do. When a receptor site is already occupied by a phytoestrogen, xenoestrogens can't attach to it. However, phytoestrogens may not stimulate the receptor causing a lower estrogenic effect. Lignans appear to be especially protective against breast cancer. One study found that women with the highest amount of dietary lignans had a 17 percent lower risk of developing breast cancer. Best protection: sprinkle ground flaxseeds over yogurt, add them to smoothies, stir them into cooked whole grains.
LENTILS are high in soluble fiber, which works as an estrogen-disposal system, says Michaels. Estrogen and xenoestrogens are normally pulled from the bloodstream by the liver and moved to the intestines. In the intestines, fiber soaks up estrogen like a sponge and removes it from the body with other waste. Other foods high in soluble fiber include apples, barley, beans, psyllium, and oat bran. Best protection: eat lentils with curry (it contains extra-protective curcumin), sprinkle oat bran over cereal, serve barley with cooked beans.
 POMEGRANATE can help block estrogenic activity by as much as 80 percent, says Michaels, and help prevent several types of breast cancer cells from multiplying; another study found similar effects on prostate cancer cells. Best protection: add pomegranate juice to green tea, scatter pomegranate seeds over salads, or add them to yogurt. Soy contains phytoestrogens called isoflavones, compounds that mimic estrogen, but in a weaker form. These weaker estrogens then block the receptor sites so xenoestrogens can't attach, says Michaels. They don't accumulate in the body like xenoestrogens, and they're metabolized more quickly.
POMEGRANATE can help block estrogenic activity by as much as 80 percent, says Michaels, and help prevent several types of breast cancer cells from multiplying; another study found similar effects on prostate cancer cells. Best protection: add pomegranate juice to green tea, scatter pomegranate seeds over salads, or add them to yogurt. Soy contains phytoestrogens called isoflavones, compounds that mimic estrogen, but in a weaker form. These weaker estrogens then block the receptor sites so xenoestrogens can't attach, says Michaels. They don't accumulate in the body like xenoestrogens, and they're metabolized more quickly.
SOY is a double-edged sword, however, says Gittleman. Some studies have suggested that high concentrations of soy isoflavones contribute to breast cancer. In addition, soy isoflavones can disrupt normal thyroid hormone function. Eat soy in moderation, avoid concentrated soy products, such as protein powders, bars, and soymilk, and check with your doctor about soy consumption if you're at high risk for prostate, breast, or uterine cancer. Best protection: add edamame to salads, crumble cooked tempeh over brown rice, stir miso into soups.
Excerpt from Sexy Hormones, by Lorna R. Vanderhaeghe, MS
Every woman from the age of menstruation until death should be taking the following nutrients every day to protect her cervix, breasts, ovaries, and uterus, and for menstruating women, to make periods effortless. These nutrients—d-glucarate, green tea extract, curcumin, milk thistle, sulforaphane, chaste tree berry, evening primrose or borage oil, and indole-3-carbinol (discussed above)—do not contain any estrogenic compounds.
D-GLUCARATE is found in all fruits and vegetables, with the highest concentrations found in apples, grapefruit, and broccoli. It is a very important nutrient that helps detoxify excess estrogens and protects from the toxic estrogens made by the liver. This nutrient is especially important if you are taking hormones of any type. Recommended dosage: 150–300 mg per day.
GREEN TEA EXTRACT is a powerful antioxidant containing polyphenols, catechins, and flavonoids, which have been shown to be protective against estrogen-dominant conditions and related cancers, especially breast and ovarian. Green tea extract helps eliminate xenoestrogens and supports the liver in metabolizing fats and hormones. Recommended dosage: 100–200 mg per day (look for products with 60 percent polyphenols) or drink green tea throughout the day. Curcumin is the yellow pigment of turmeric, one of the chief ingredients in curry.
CURCUMIN is a powerful anti-inflammatory, and it also helps eliminate cancer-causing estrogens and environmental estrogens via the liver. Curcumin increases detoxification. Recommended dosage: 50–100 mg per day. Use the spice turmeric in cooking too.
MILK THISTLE, called the protector of the liver, is extremely important for proper estrogen balance in the cells of the body. It detoxifies a wide range of hormones, drugs, and toxins, among other things. Recommended dosage: 50–100 mg per day (ensure that your milk thistle contains at least 80 percent silymarin, an active ingredient in the herb).
SULFORAPHANE from broccoli sprout extract has been shown to stimulate the body's production of detoxification enzymes that eliminate toxic estrogens and balance estrogens in the body. Recommended dosage: 200–400 mcg per day.
VITEX (chaste tree berry), also called the progesterone-enhancing herb, contains no hormones, has no direct hormonal activity, and is not phytoestrogenic. Its main active ingredients work on the pituitary gland to stimulate the production of luteinizing hormone, which in turn increases progesterone and helps regulate the menstrual cycle. It is recommended for irregular or heavy periods, cramps, polycystic ovary syndrome, PMS, breast tenderness, bloating, depression and mood swings, reduction of ovarian cysts, acne related to hormonal imbalance, infertility, endometriosis, and many other female-related symptoms. Recommended dosage: 2–4 capsules per day with food.
EVENING PRIMROSE, BORAGE, andBLACK CURRENT SEED OIL are classified as "good" omega-6 oils and have been shown in clinical studies to be breast-cancer protective. GLA is known to ease cramps and breast pain, and reduce PMS, depression, and bloating. Recommended dosage: 4,000 mg of borage oil or 8,000 mg of evening primrose oil, every day with food.

Photo: Hotze Wellness